If you’ve recently been told you have “degenerative disc disease,” you might be feeling rather worried. The word “disease” sounds frightening, doesn’t it? It conjures images of progressive deterioration and inevitable disability. But here’s something that might surprise you: degenerative disc disease isn’t actually a disease at all, and having it doesn’t mean you’re destined for a life of chronic pain.
As a chiropractic clinic in Brighton, we see patients every week who’ve been given this diagnosis and are understandably concerned. The good news? Modern research paints a far more optimistic picture than you might think. So what’s really happening in your spine and, more importantly, what can you actually do about it?
What Is Degenerative Disc Disease?
Despite its ominous name, degenerative disc disease (DDD) is simply the medical term for the natural wear and tear that occurs in the cushioning discs between your vertebrae as you age. Think of it less as a “disease” and more like getting grey hair or wrinkles – it’s a normal part of getting older.
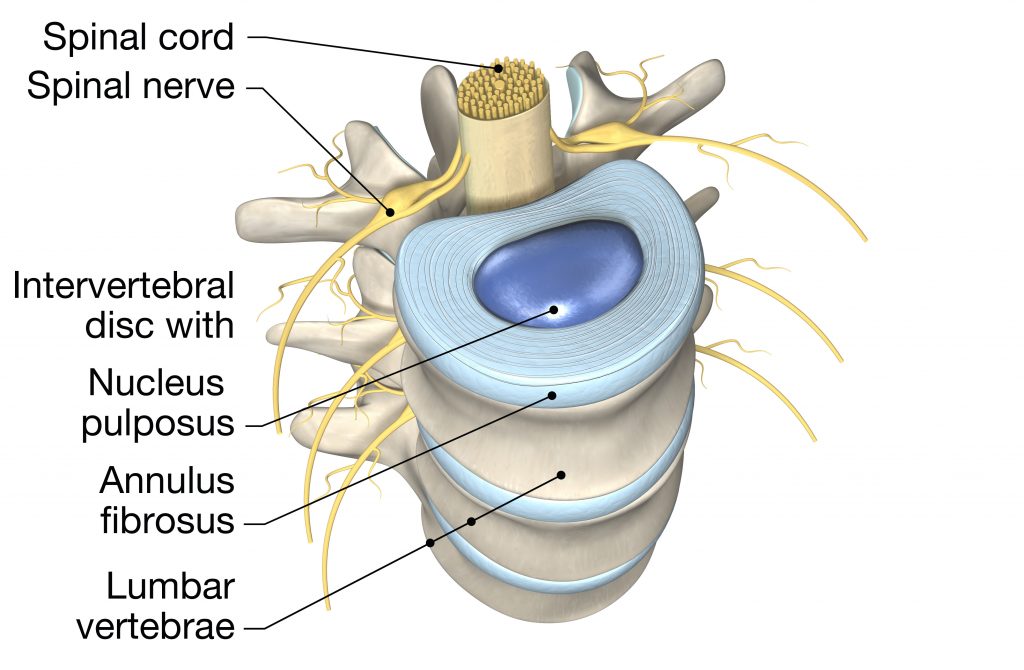
Your spinal discs are remarkable structures. They act like shock absorbers, with a tough outer layer (the annulus fibrosus) surrounding a gel-like centre (the nucleus pulposus). These discs allow your spine to bend, twist and absorb the impact of daily activities.
From around your 30s onwards, these discs naturally begin to change. They lose some of their water content, becoming slightly less plump and flexible. The outer layers may develop small tears, and the overall height of the disc can decrease. This is what radiologists see on MRI scans when they report “degenerative disc disease.”
Here’s the Crucial Bit: Disc Degeneration Doesn’t Equal Pain
This is where the research gets really interesting – and reassuring. A landmark 2015 study published in the American Journal of Neuroradiology examined MRI scans of over 3,000 people without any back pain whatsoever. The findings were remarkable:
- 37% of 20-year-olds showed disc degeneration
- 52% of 30-year-olds had degenerative changes
- 68% of 40-year-olds showed signs of disc degeneration
- 80% of 50-year-olds had degenerative disc changes
- 96% of 80-year-olds showed disc degeneration
Let that sink in for a moment. The vast majority of these individuals had “degenerative disc disease” on their scans but felt absolutely fine. They had no back pain, no symptoms and were going about their daily lives without any problems.
This research, along with numerous other studies, shows us something vital: disc degeneration is incredibly common in pain-free individuals and is simply a normal part of ageing.
A 2020 review in The Lancet confirmed that “imaging findings of degenerative changes in the spine are poorly correlated with pain and disability.” In other words, what shows up on your scan often has very little to do with how you actually feel.
So Why Does My Back Hurt?
If degenerative discs are normal and often pain-free, why do some people experience back pain? This is where things get more complex – and more hopeful.
Research from the past decade has revolutionised our understanding of back pain. We now know that pain is influenced by multiple factors:
Physical factors such as how you move, your muscle strength and flexibility, and yes, sometimes the degree of disc changes can play a role – but it’s rarely the whole story.
Lifestyle factors including your activity levels, sleep quality, and general fitness have a significant impact on back pain.
Psychological factors such as stress, anxiety, fear of movement and previous pain experiences can amplify or reduce pain signals.
Social factors including job satisfaction, financial stress and social support networks also influence how we experience pain.
A 2018 study in JAMA Internal Medicine found that fear avoidance – being afraid to move because you think you’ll cause more damage – is actually one of the strongest predictors of chronic back pain. The good news? This is something we can address.
Why “Disease” Is the Wrong Word
The medical community is increasingly recognising that calling this condition a “disease” is misleading and potentially harmful. Here’s why:
- It’s universal: nearly everyone develops disc degeneration if they live long enough. We don’t call wrinkled skin a disease.
- It’s often asymptomatic: most people with disc degeneration have no pain at all.
- It’s not progressive like a disease: DDD doesn’t necessarily worsen over time, and many people’s symptoms improve despite their discs remaining the same.
- The label can cause harm: research shows that scary-sounding diagnoses can actually make pain worse through a phenomenon called “nocebo effect” – the opposite of placebo. When people believe they have a serious disease, they may become fearful of movement and more disabled than the physical changes would warrant.
Leading pain researchers have argued that we should stop using the term “degenerative disc disease” altogether and instead talk about “age-related disc changes” – a far more accurate and less frightening description.
Evidence-Based Management: What Actually Helps?
Now for the really good news: there’s strong evidence for several effective approaches to managing back pain associated with disc changes. At Sundial Brighton, these are the strategies we recommend based on current research:
1. Stay Active and Keep Moving
This is perhaps the most important message. A 2017 systematic review in the British Journal of Sports Medicine found that exercise therapy is one of the most effective treatments for chronic low back pain.
The type of exercise matters less than simply being active. Walking, swimming, yoga, Pilates, strength training – all have evidence supporting their use. The key is finding activities you enjoy and can stick with.
Contrary to old beliefs, movement doesn’t “wear out” your discs further. In fact, controlled movement helps maintain disc health by pumping nutrients into the disc tissue.
2. Targeted Exercises and Rehabilitation
Whilst general activity is crucial, specific exercises can be particularly helpful. Research from 2019 in The Spine Journal showed that exercises targeting the following areas can significantly reduce pain and improve function:
- Core stability (the deep muscles that support your spine)
- Hip and gluteal strength (to reduce strain on your lower back)
- Flexibility and mobility work
Sundial chiropractors can assess your individual movement patterns and prescribe exercises tailored to your specific needs, addressing any weakness or stiffness that might be contributing to your pain.
3. Manual Therapy and Chiropractic Care
Chiropractic treatment, including spinal manipulation and mobilisation, has good evidence for managing back pain. A 2017 systematic review found that spinal manipulation is an effective treatment and can be particularly effective when combined with exercise.
How manual therapy works:
- Reduces muscle tension and improves joint mobility
- Provides pain relief through neurological mechanisms
- Helps restore normal movement patterns
- Gives you confidence to move more freely
It’s important to note that chiropractic care doesn’t “reverse” disc degeneration – nothing can do that. Instead, it addresses the factors that contribute to pain and helps your body function better despite the age-related changes in your discs.
4. Pain Education and Changing Your Understanding
This might sound simple, but research consistently shows that understanding pain can reduce it. A 2018 study in Clinical Rehabilitation found that pain neuroscience education – learning about how pain actually works – significantly reduced pain and disability in people with chronic back pain.
Understanding these key points can be genuinely therapeutic:
- Your discs aren’t “crumbling” or “deteriorating” in a disease-like way
- Pain doesn’t necessarily mean damage
- Movement is safe and beneficial, not harmful
- Your prognosis is generally good
This knowledge helps reduce fear and allows you to become more active, which in itself reduces pain.
5. Lifestyle Modifications
The evidence increasingly shows that general health significantly impacts back pain:
Sleep. Poor sleep is strongly associated with increased pain. A 2019 study in PAIN journal found that improving sleep quality can reduce back pain severity.
Stress management. Chronic stress amplifies pain signals. Techniques like mindfulness, meditation, or simply finding time for activities you enjoy can help.
Healthy weight. Whilst there’s no need to be stick-thin, maintaining a healthy weight reduces mechanical load on your spine and decreases inflammatory markers associated with pain.
Smoking cessation. Smoking reduces blood flow to spinal tissues and is associated with worse back pain outcomes. It’s worth getting support to quit if you smoke.
6. Addressing Psychological Factors
This isn’t about pain being “all in your head” – it’s about recognising that our thoughts and emotions genuinely influence our pain experience. Research from 2020 in The Journal of Pain showed that cognitive behavioural therapy (CBT) approaches can be as effective as physical treatments for chronic back pain.
A good chiropractor will consider these factors as part of your care, possibly advising you to seek help from appropriate professionals if needed.
What About Advanced Treatments?
You might be wondering about injections, surgery, or other interventions. The research here is quite clear: for most people with degenerative disc disease, conservative management (the approaches listed above) should be tried first and continued for at least 12 weeks.
A 2016 study in The BMJ compared surgery with intensive rehabilitation for people with degenerative disc disease. Two years later, both groups had similar outcomes – but the rehabilitation group avoided surgical risks and costs.
Surgery has a role in specific circumstances, particularly when there’s nerve compression causing significant leg symptoms. However, for typical back pain associated with disc degeneration, surgery rarely outperforms conservative care.
Your Action Plan: What to Do Next
If you’ve been diagnosed with degenerative disc disease, here’s your evidence-based action plan:
Immediate steps:
- Take a deep breath and remember: this is normal age-related change, not a progressive disease
- Stay as active as possible within your comfort zone
- Avoid bed rest (more than a day or two can actually make things worse)
- Use pain relief if needed – it can help you stay active
Short-term (first few weeks):
- Make an appointment with one of our chiropractors at Sundial for an assessment and advice on movement
- Begin gentle exercises – even just walking 20 minutes daily
- Apply heat or cold (whichever feels better to you)
- Address any fear or worry about your diagnosis through education
Long-term (ongoing):
- Develop a regular exercise routine you enjoy
- Build strength progressively, particularly in your core and legs
- Manage stress and prioritise sleep
- Stay educated about pain – knowledge is power
The Brighton Perspective: Getting Local Support
Here in Brighton, we’re fortunate to have excellent resources for managing back pain. Beyond chiropractic care, you might consider:
- Local swimming pools (the sea if you’re brave!) for low-impact exercise
- Yoga and Pilates studios throughout the city
- Walking routes along the seafront or in the Downs
- Gyms with knowledgeable trainers who can guide your strength work (we have a small on-site gym and personal trainer at our St James’s Street branch).
The key is finding support that fits your lifestyle and preferences. Here at Sundial our chiropractors make sure that they:
- Take time to explain your condition clearly
- Provide evidence-based care
- Emphasise active approaches and self-management
- Work collaboratively with Sundial physiotherapists and massage therapists if needed
The Bottom Line: It Really Isn’t All Bad News
Degenerative disc disease sounds frightening, but the research is clear: it’s a normal part of ageing that doesn’t doom you to a life of pain and disability. Most people with degenerative changes on their scans feel absolutely fine, and those who do experience pain have excellent options for evidence-based management.
If you’re struggling with back pain and concerned about degenerative disc disease, don’t let fear hold you back from living your life. Your spine is remarkably resilient, and with the right approach, there’s every reason to expect you’ll feel better and continue doing the things you love – grey hair, wrinkles, degenerative discs and all.
If you’re experiencing back pain and would like an evidence-based assessment and treatment plan, our chiropractic clinics in Brighton are here to help. We focus on empowering you with knowledge, movement, and strategies that actually work – based on the latest research, not outdated fears about your spine.
Frequently Asked Questions About Degenerative Disc Disease
Is degenerative disc disease serious?
No, degenerative disc disease is not a serious disease despite its alarming name. It’s simply the medical term for normal age-related changes in your spinal discs. Research shows that 80% of 50-year-olds have degenerative disc changes on scans but no symptoms. It’s similar to getting grey hair – a natural part of ageing rather than a medical condition requiring alarm.
Can you live a normal life with degenerative disc disease?
Yes, absolutely. The vast majority of people with degenerative disc disease live completely normal, active lives. Studies show that disc degeneration is incredibly common in pain-free individuals. With appropriate management including exercise, chiropractic care, and lifestyle modifications, most people can continue all their usual activities without significant limitations.
What should you not do with degenerative disc disease?
The most important thing NOT to do is avoid movement out of fear. Bed rest beyond a day or two can actually make things worse. Avoid catastrophic thinking about your diagnosis and don’t let fear prevent you from staying active. There’s no evidence that normal daily activities or exercise will damage your discs further – in fact, movement helps maintain disc health.
Does degenerative disc disease get worse with age?
Not necessarily. Whilst disc degeneration is age-related, it doesn’t follow a predictable downward path. Many people’s symptoms improve over time despite their discs remaining unchanged on scans. The condition doesn’t behave like a progressive disease – pain levels often fluctuate and can improve significantly with appropriate management, regardless of what shows on imaging.
What is the best treatment for degenerative disc disease?
Research shows that a combination of approaches works best: staying active with regular exercise, targeted strengthening and flexibility work, manual therapy such as chiropractic care, pain education, and lifestyle modifications including good sleep and stress management. A 2016 study in The BMJ found that intensive rehabilitation produces similar outcomes to surgery but without the risks. Conservative management should always be tried first.
Can a chiropractor help with degenerative disc disease?
Yes, chiropractors can help manage symptoms associated with degenerative disc disease. Research shows that spinal manipulation and mobilisation, combined with exercise prescription and education, can significantly reduce pain and improve function. A chiropractor in Brighton can assess your individual movement patterns, provide manual therapy to reduce muscle tension and improve mobility, and develop a personalised exercise programme. Chiropractic care doesn’t reverse disc degeneration but addresses the factors contributing to pain.
How long does degenerative disc disease last?
This question reflects a misunderstanding of the condition. Degenerative disc changes are permanent age-related changes to your spinal structure – they don’t “go away.” However, pain associated with these changes is often temporary and episodic. Most people experience improvement within 12 weeks with appropriate management. The key point is that disc degeneration and pain are separate issues – you can have degenerative changes permanently but be pain-free.
What percentage of people have degenerative disc disease?
According to a landmark 2015 study in the American Journal of Neuroradiology, degenerative disc changes are extremely common in symptom-free individuals: 37% of 20-year-olds, 52% of 30-year-olds, 68% of 40-year-olds, 80% of 50-year-olds, and 96% of 80-year-olds show disc degeneration on MRI scans. This demonstrates that it’s a normal part of ageing rather than a disease.
Should I avoid exercise with degenerative disc disease?
No, you should not avoid exercise. Exercise is one of the most effective treatments for back pain associated with disc degeneration. A 2017 systematic review in the British Journal of Sports Medicine confirmed that exercise therapy is highly effective for chronic low back pain. Movement helps pump nutrients into disc tissue and maintains spinal health. The type of exercise matters less than staying consistently active – walking, swimming, yoga, Pilates, and strength training all have supporting evidence.
When should I see a chiropractor for degenerative disc disease?
Consider seeing a chiropractor in Brighton if you’re experiencing back pain that’s affecting your daily activities, if you’re unsure how to exercise safely, or if you want professional guidance on managing your symptoms. Early intervention can prevent fear avoidance behaviours and help you develop effective self-management strategies. You should seek urgent medical attention if you experience progressive leg weakness, loss of bladder or bowel control, or severe unrelenting pain – though these symptoms are rare with typical degenerative disc disease.
About Matthew Bennett, Chiropractor Brighton
Matthew Bennett is the founder and principal chiropractor at Sundial Clinics Brighton, established in 1991. With over 35 years of clinical experience, Matthew qualified from the Anglo-European College of Chiropractic in 1987 and served as President of the British Chiropractic Association for four years. As a Fellow of the Royal College of Chiropractors and former team chiropractor for Brighton and Hove Albion FC and the British Alpine Ski Team, Matthew combines evidence-based chiropractic treatment with sports performance expertise. His authority in musculoskeletal health has been recognised through national media appearances, expert witness roles and contributions to professional publications. Matthew’s commitment to clinical excellence ensures patients receive the most effective chiropractic care in Brighton.
